Focus on consistent, alternating leg movements. This ensures efficient locomotion and minimizes energy expenditure. Aim for a smooth, rhythmic pattern, avoiding jerky or uneven steps. This improves balance and reduces the risk of falls.
Proper reciprocal gait requires strong hip flexors and extensors. Strengthen these muscle groups through exercises like lunges, squats, and bridges. Include regular cardiovascular training to improve overall endurance and stamina, directly impacting gait performance. Aim for at least 150 minutes of moderate-intensity cardio per week.
Observe your gait in a mirror or video recording. Identify asymmetries or deviations from a smooth, alternating pattern. Address any imbalances through targeted physical therapy or exercises. Consult a physical therapist for personalized recommendations based on your specific needs and any existing conditions.
Note: Regular assessment by a healthcare professional is vital for monitoring progress and adjusting your training plan. They can provide valuable feedback and ensure your exercises are tailored to your abilities and goals, avoiding potential injury.
- Reciprocal Gait Pattern: A Detailed Overview
- Defining Reciprocal Gait: What it is and why it’s important
- Neural Control of Reciprocal Gait: The role of central pattern generators
- Muscular Coordination in Reciprocal Gait: Antagonistic muscle interaction
- The Role of Sensory Feedback
- Training Implications
- Biomechanics of Reciprocal Gait: Understanding limb movements and joint angles
- Factors Affecting Reciprocal Gait: Speed, terrain, and fatigue
- Developmental Aspects of Reciprocal Gait: From infancy to adulthood
- Clinical Implications of Altered Reciprocal Gait: Identifying and treating gait disorders
- Identifying Gait Disorders
- Treating Gait Disorders
- Technological Applications in Gait Analysis: Measuring and improving reciprocal gait
- Motion Capture Systems
- Force Plates and Pressure Mapping
- Machine Learning Applications
- Virtual Reality and Robotics
- Biomechanical Modeling
- Reciprocal Gait in Other Animals: Comparative perspectives
Reciprocal Gait Pattern: A Detailed Overview
Observe the alternating movement of limbs: one leg moves forward while the opposite leg moves backward. This is the core principle of reciprocal gait. This pattern, crucial for locomotion in many animals, ensures stability and efficiency.
Neural Control: Central pattern generators (CPGs) in the spinal cord orchestrate this rhythmic coordination. Sensory feedback from limbs refines the pattern, adapting to the terrain and speed.
Factors Affecting Gait: Several elements influence the reciprocal gait pattern’s execution. These include muscle strength, joint flexibility, and neurological integrity. Injuries or diseases can disrupt this pattern, leading to abnormal gaits.
Clinical Relevance: Assessing gait is vital for diagnosing neurological disorders. Variations in reciprocal gait can indicate problems like spinal cord injury, stroke, or cerebral palsy. Gait analysis tools help quantify these variations for precise diagnosis and treatment planning.
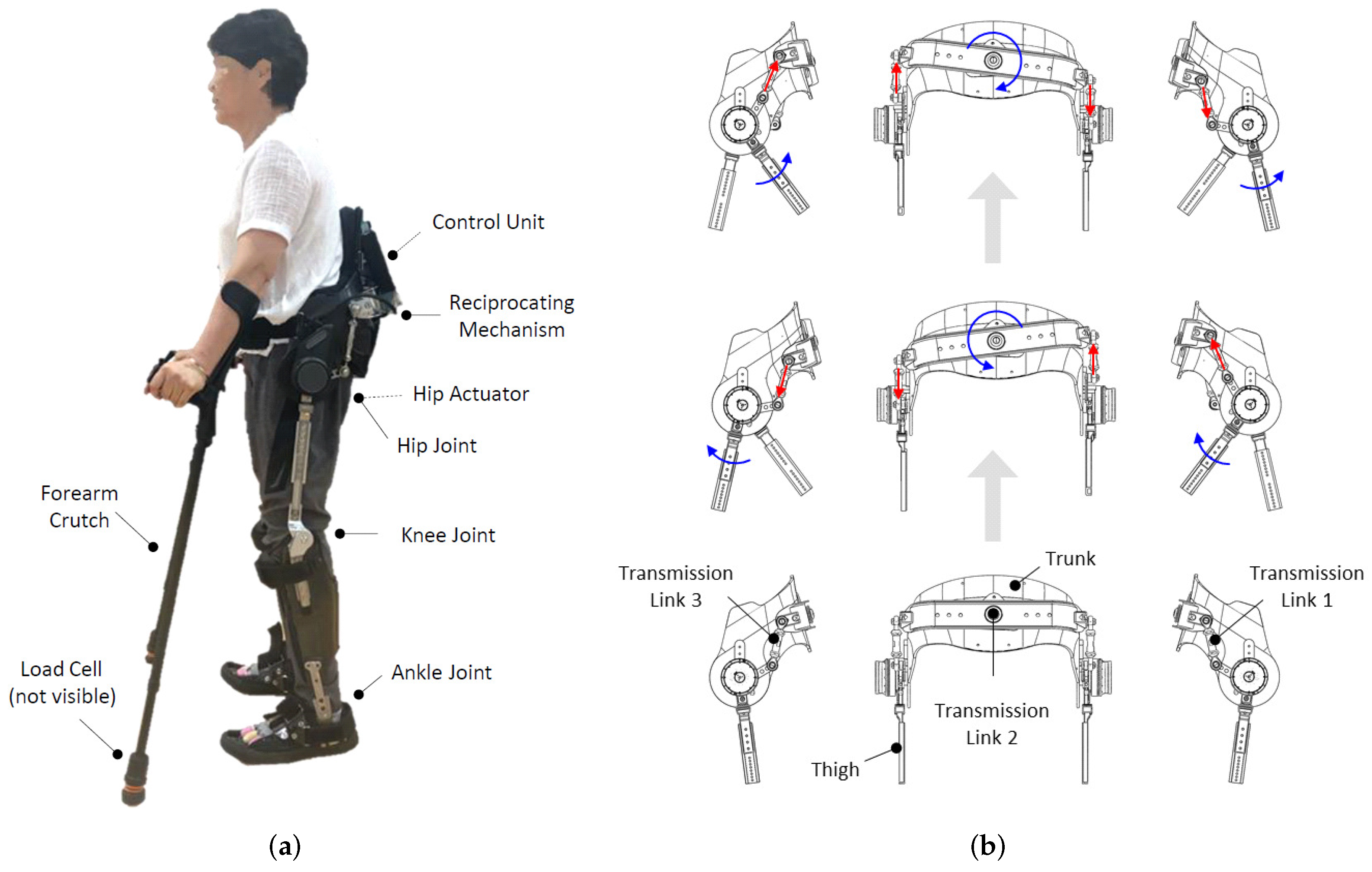
Therapeutic Interventions: Physical therapy plays a crucial role in restoring or improving reciprocal gait. Targeted exercises strengthen muscles, improve flexibility, and retrain neural pathways involved in locomotion. Robotics and assistive devices may also aid in rehabilitation.
Examples in Nature: From insects to mammals, variations of reciprocal gait exist, each adapted to specific environments and needs. Studying these diverse implementations provides valuable insights into the mechanics and evolution of locomotion.
Further Research: Current research focuses on advanced gait analysis techniques, improved prosthetic design to enhance reciprocal gait, and a deeper understanding of CPGs. These advancements promise better diagnostic tools and more effective rehabilitation strategies.
Defining Reciprocal Gait: What it is and why it’s important
Reciprocal gait refers to the alternating movement of limbs during locomotion. Think of walking: one leg moves forward while the other supports your weight, then they switch. This coordinated pattern is fundamental for efficient and stable movement.
Understanding reciprocal gait is critical for several reasons. First, it forms the basis for analyzing various gaits in different animals, from insects to humans. This comparison reveals evolutionary adaptations and biomechanical principles. Secondly, it’s crucial for diagnosing and treating gait disorders. Analyzing deviations from the typical reciprocal pattern helps identify neurological or musculoskeletal problems.
For example, observing an asymmetrical gait–where one leg swings differently than the other–can indicate a muscle imbalance, nerve damage, or joint injury. Early detection via gait analysis enables timely intervention and improved patient outcomes. Furthermore, understanding the mechanics of reciprocal gait informs the design of prosthetic limbs and assistive devices, ensuring optimal functionality and minimizing energy expenditure.
Finally, reciprocal gait research contributes to robotics. Mimicking this natural pattern allows for the creation of more efficient and stable walking robots, with potential applications in various fields, such as search and rescue operations and exploration in challenging terrains.
Neural Control of Reciprocal Gait: The role of central pattern generators
Central pattern generators (CPGs) are neural circuits within the spinal cord that produce rhythmic motor patterns without continuous sensory feedback. They are the key to understanding reciprocal gait.
Think of CPGs as the body’s built-in walking machine. They generate the alternating flexion and extension of limbs required for locomotion. This inherent rhythmicity allows for basic walking even without higher brain input. The precise timing and coordination, however, are refined by sensory feedback.
- Half-center organization: Many CPGs use a “half-center” model. Two interconnected neuronal populations inhibit each other, creating the alternating activity needed for reciprocal movement. One population drives flexion, the other extension. This reciprocal inhibition is crucial.
- Sensory feedback: While CPGs initiate the rhythmic pattern, sensory input constantly adjusts the gait. Proprioceptors in muscles and joints provide information about limb position and muscle length. This feedback modifies the CPG output for adjustments to speed, terrain, and obstacles.
- Modulation from supraspinal centers: Higher brain centers, such as the brainstem and cortex, modulate CPG activity. They influence gait speed, direction, and adapt the walking pattern to complex environments. This higher-level control ensures adaptability and allows for sophisticated movement. For example, the mesencephalic locomotor region (MLR) in the brainstem plays a key role in initiating and controlling locomotion.
Research on CPGs uses various techniques. Electrophysiological recordings from spinal cord neurons directly measure the activity of CPGs during locomotion. Computational modeling allows for testing hypotheses about network interactions within CPGs. Studying animal models, especially those with spinal cord injuries, clarifies the role of CPGs in locomotion and rehabilitation strategies.
- Understanding CPGs is critical for developing effective rehabilitation therapies for spinal cord injuries.
- CPG-based neuroprostheses aim to restore locomotion by electrically stimulating the spinal cord, mimicking natural CPG activity.
- Further research into CPGs may lead to new treatments for neurological disorders affecting gait.
Muscular Coordination in Reciprocal Gait: Antagonistic muscle interaction
Proper reciprocal gait relies on precise interplay between agonist and antagonist muscles. Agonist muscles, like the tibialis anterior (dorsiflexion) and hamstrings (flexion), initiate movement. Simultaneously, antagonist muscles, such as the gastrocnemius (plantarflexion) and quadriceps (extension), control the speed and range of that movement through a process called reciprocal inhibition. This inhibition, mediated by the nervous system, prevents antagonist muscles from opposing the agonist’s action too forcefully, leading to smooth, coordinated locomotion. Effective reciprocal inhibition requires properly functioning sensory feedback loops, conveying information about limb position and muscle length. This constant feedback loop allows the nervous system to fine-tune muscle activation.
The Role of Sensory Feedback
Proprioceptors, such as muscle spindles and Golgi tendon organs, play a critical role. Muscle spindles monitor muscle length and rate of change, triggering reflex adjustments in muscle activation. Golgi tendon organs detect muscle tension, protecting against excessive force. Dysfunction in these sensory systems can disrupt reciprocal inhibition, resulting in uncoordinated movement or gait abnormalities. Consider the impact of a damaged muscle spindle: the nervous system might receive inaccurate information about muscle length, leading to an inappropriate level of antagonist activation, manifesting as stiffness or jerky movements.
Training Implications
Targeted exercises improve reciprocal inhibition. For instance, activities emphasizing controlled movements and proprioceptive awareness, like balance exercises or specific stretching routines that target both agonists and antagonists, enhance neuromuscular coordination. Focus on exercises that gradually increase the range of motion while maintaining control to avoid overstretching and injury. Regular physical activity maintains optimal muscle tone and improves the communication between muscles and the nervous system. This improves the precision and efficiency of the reciprocal gait pattern.
Biomechanics of Reciprocal Gait: Understanding limb movements and joint angles
Analyze reciprocal gait by focusing on the interplay between limb movements and joint angles. Observe the swing and stance phases of each leg.
During the swing phase, hip flexion initiates the leg’s forward movement. Knee flexion further contributes to leg advancement, clearing the ground. Ankle dorsiflexion helps the foot clear the ground. Typical ranges are: hip flexion 30-60°, knee flexion 60-90°, and ankle dorsiflexion 10-20°. These values vary with stride length and walking speed.
The stance phase involves controlled joint extension. Hip extension stabilizes the body. Knee extension bears weight and propels the body forward. Ankle plantarflexion provides propulsion at push-off. Typical ranges are: hip extension 0-10°, knee extension from flexion to full extension, and ankle plantarflexion 20-40°.
Arm swing complements leg movement, creating counter-rotation for balance. Observe the oppositional arm swing – as the right leg advances, the left arm swings forward. This involves shoulder and elbow joint flexion and extension. Analysis should note the phase relationship between arm and leg movements.
| Phase | Joint | Movement | Approximate Angle Range (degrees) |
|---|---|---|---|
| Swing | Hip | Flexion | 30-60 |
| Swing | Knee | Flexion | 60-90 |
| Swing | Ankle | Dorsiflexion | 10-20 |
| Stance | Hip | Extension | 0-10 |
| Stance | Knee | Extension | 0-180 |
| Stance | Ankle | Plantarflexion | 20-40 |
Remember these values are approximations. Individual variations exist due to factors like age, gait speed, and underlying conditions. Accurate measurement requires gait analysis equipment. Detailed kinematic data provides more precise descriptions of limb and joint behavior.
Factors Affecting Reciprocal Gait: Speed, terrain, and fatigue
Increased walking speed significantly alters reciprocal gait. Studies show a decrease in swing phase duration and an increase in stride frequency above 1.2 m/s. This speed adjustment prioritizes coverage of ground rather than detailed foot placement.
Uneven terrain demands adjustments. Rough or inclined surfaces necessitate shorter strides and increased ground reaction force, impacting both the stance and swing phases. A study by Winter (1991) demonstrated a 20% increase in muscle activity on uneven surfaces.
Fatigue profoundly modifies reciprocal gait. Prolonged walking leads to altered muscle activation patterns, resulting in reduced stride length and frequency. A study in the *Journal of Applied Physiology* showed a 15% decrease in stride length after 60 minutes of continuous walking on a treadmill at moderate speed. This often manifests as a wider base of support and slower cadence.
Developmental Aspects of Reciprocal Gait: From infancy to adulthood
Observe infants’ stepping reflex: Around 2 months old, babies show this reflex when held upright. This spontaneous stepping illustrates the early presence of neural pathways supporting reciprocal gait. However, true independent walking requires significant maturation.
Between 9 and 15 months, most toddlers begin walking. Initially, their gait is characterized by wide base of support, short steps, and high variability. They achieve mature gait by 3-5 years, with a more stable, coordinated pattern. This includes a smoother walking rhythm and longer stride length.
During childhood and adolescence, gait continues refining. Increased leg length and improved balance contribute to greater speed and efficiency. The gait cycle becomes more fluid, with a more pronounced heel strike.
In adulthood, gait changes gradually. Age-related decline in muscle strength and joint flexibility might lead to slower walking speed, shorter stride length, and decreased stability. However, this varies greatly depending on individual health and activity levels. Regular exercise significantly mitigates age-related gait deterioration.
Understanding these developmental stages helps clinicians identify potential gait abnormalities early. Interventions, such as physical therapy, can address issues like cerebral palsy or other neurological conditions, improving gait and overall mobility across the lifespan.
Clinical Implications of Altered Reciprocal Gait: Identifying and treating gait disorders
Assess gait deviations using validated scales like the Gait Deviation Index (GDI) or the Timed Up and Go (TUG) test. These provide objective measures for comparison and tracking progress.
Identifying Gait Disorders
- Observe the patient’s gait: Note asymmetry in step length, stride time, and base of support. Look for deviations in posture, arm swing, and foot placement.
- Analyze muscle strength and tone: Weakness in hip flexors, extensors, or ankle muscles significantly impacts reciprocal gait. Increased muscle tone (spasticity) can also hinder smooth movement. Use manual muscle testing and electromyography (EMG) for a thorough evaluation.
- Assess joint range of motion (ROM): Limited ROM in hips, knees, or ankles restricts normal gait mechanics. Goniometry measures the extent of joint movement.
- Evaluate sensory input: Sensory impairments, such as proprioception loss, negatively affect gait control. Conduct sensory tests to assess proprioception, vibration, and touch.
- Consider neurological factors: Neurological conditions like stroke, Parkinson’s disease, and multiple sclerosis frequently cause gait abnormalities. A neurological examination is crucial.
Treating Gait Disorders
Treatment strategies depend on the underlying cause of the gait disorder. A multidisciplinary approach is often most beneficial.
- Physical therapy: Focuses on strengthening weakened muscles, improving ROM, and retraining gait patterns. Techniques include targeted exercises, gait training, and the use of assistive devices (canes, walkers).
- Occupational therapy: Addresses functional limitations and improves activities of daily living. This may involve adaptive equipment or environmental modifications.
- Pharmacological interventions: Medications can manage spasticity, pain, and other symptoms. Botulinum toxin injections may reduce muscle tone.
- Surgical interventions: In severe cases, surgery may correct anatomical abnormalities or address specific musculoskeletal issues.
- Assistive devices: These help improve mobility, balance, and stability. Examples include orthoses, canes, walkers, and wheelchairs.
Regular follow-up appointments are needed to monitor progress, adjust treatment plans, and prevent recurrence. Patient education plays a critical role in adherence and successful management of gait disorders. Encourage patients to actively participate in their rehabilitation plan.
Technological Applications in Gait Analysis: Measuring and improving reciprocal gait
Accelerometers and gyroscopes embedded in wearable sensors provide real-time data on joint angles, movement speed, and step length, offering precise reciprocal gait measurements. This data allows clinicians to identify asymmetries and deviations from a normal gait pattern, enabling early diagnosis of gait disorders.
Motion Capture Systems
High-speed cameras and infrared systems capture 3D movement, generating detailed visualizations of the entire body’s motion during gait. This level of detail reveals subtle nuances in reciprocal gait, helping clinicians understand the interplay between different body segments. Expect accuracy within a millimeter or better in advanced systems. Combine these visual data with force plate information for even greater precision.
Force Plates and Pressure Mapping
Force plates measure ground reaction forces, providing insights into the forces exerted during each phase of the gait cycle. This quantifies weight-bearing distribution, identifying potential issues in gait symmetry and efficiency. Pressure mapping systems offer even more detailed analysis, showing pressure distribution across the foot throughout the gait cycle, which is valuable for identifying plantar pressure abnormalities.
Machine Learning Applications
Machine learning algorithms analyze gait data, identifying patterns and predicting potential risks. This allows for personalized interventions and proactive management of gait disorders. For example, these algorithms can recognize subtle changes indicating a possible fall risk, prompting early intervention. Advanced models can even predict future gait deterioration based on current data trends.
Virtual Reality and Robotics
VR systems create immersive environments for gait rehabilitation, allowing patients to practice walking in challenging and controlled conditions. Robotic exoskeletons provide physical support and assistance, guiding patients through targeted movements and improving their gait pattern. These technologies offer a tailored approach, improving patient engagement and rehabilitation outcomes.
Biomechanical Modeling
Computational models simulate gait mechanics, predicting the effects of interventions and optimizing rehabilitation plans. This personalized approach helps healthcare providers make informed decisions about treatment strategies based on patient-specific data.
Reciprocal Gait in Other Animals: Comparative perspectives
Observe how diverse animals utilize reciprocal gait. Quadrupeds, like horses and dogs, often employ a diagonal gait, coordinating legs diagonally opposite each other for efficient locomotion. This differs from the lateral sequence seen in many reptiles, where legs on the same side move together.
Birds, surprisingly, display a variety of gaits. While walking, many demonstrate a reciprocal pattern, alternating legs. However, running birds often shift to a more complex gait involving lateral sequences or even bounding.
Insects provide a fascinating case study. Most insects use a tripod gait, where three legs support the body while the other three move. Although not strictly reciprocal in the same way as vertebrates, this still maintains a rhythmic, alternating pattern of leg movement.
Consider cephalopods, like octopuses. Their locomotion utilizes jet propulsion primarily, but they also demonstrate reciprocal movement of their arms during crawling, often coordinating pairs of arms for efficient grip and propulsion.
Studying these variations reveals how gait adaptations reflect the animal’s morphology, environment, and evolutionary history. Researchers comparing reciprocal gait across species frequently focus on muscle coordination, limb morphology, and energetic efficiency to uncover the underlying principles governing locomotion.
Further research should explore the neural control of reciprocal gait in different species, examining how central pattern generators differ across taxa. This comparative approach could illuminate the evolution of sophisticated locomotor control systems.